|
This discrepancy could occur due to the different effect of PEEP in patients with various degrees of lung injury or, in positive PEEP responders, the reduction in alveolar dead space compensated for the concurrent increase in airway dead space. 
In some studies in patients with ARDS, adequate PEEP corresponded to the lowest VD/VTphys and to the lowest arterial to end-tidal PCO 2 gradient PEEP levels also correlated well with the extent of quantitatively measured lung inhomogeneities assessed on computed tomography (CT) images of the lung. In ARDS, ideal PEEP titration achieves a balance between maintaining optimal alveolar recruitment and reasonably avoiding lung overdistension. Whether VD/VTphys is useful for PEEP titration is a matter of debate. found that VD/VTphys measurement using CO 2 production estimated from the Harris-Benedict equation predicted mortality in patients with acute lung injury (ALI) in a dose-response manner. Moreover, during the first 2 days of ARDS, the evolution of noninvasive capnographic indices such as the ratio between alveolar ejection volume and VT, which can be calculated without arterial blood gas sampling, has a prognostic value similar to VD/VTphys. Other groups found similar results in early and intermediate phases of ARDS and in patients with ARDS according to the Berlin definition undergoing lung-protective ventilation. demonstrated that a high VD/VTphys was independently associated with an increased risk of death in patients with ARDS. Although the Enghoff approach to calculating VD/VTphys can be contaminated by the large shunt fractions present in ARDS, the result is a good global index of the efficiency of the gas exchange of a lung. Since VD/VTphys reflects alterations in V/Q ratios, it is affected by any type of V/Q mismatch. In ARDS, alveolar and endothelial cell injuries result in alterations of the pulmonary microcirculation in all lung compartments with high and low ventilation/perfusion (V/Q) ratios. First, dead space has important prognostic implications. There are several reasons why dead space is an attractive parameter that should be routinely monitored in critical care. Factors that explain this reluctance to monitor dead space at the bedside include difficulties in understanding physiologically derived information and in interpreting capnograms, together with the lack of integration of CO 2 waveforms and derived data with other respiratory measurements. Unfortunately, in critical care practice dead space is not routinely measured at the bedside. This is, in a nutshell, exactly what intensivists strive for at the bedside: to recruit the lung without doing harm. The authors state that “this observation supports the concept of the recruitment of previously atelectatic lung areas leading to an increase in compliance and a decrease in alveolar dead space, whereas overdistension of alveoli decreases compliance and increases alveolar dead space”. Interestingly, the decrease in VD/VTphys occurred with no significant change in anatomic dead space. 
Although they used the maximum level of oxygen transport to determine the optimum levels of PEEP, they showed that maximizing total compliance and minimizing physiologic dead space (VD/VTphys) yielded the best results. pointed out that increasing positive end-expiratory pressure (PEEP) in ARDS augments blood oxygenation and decreases shunt. However, if data generated breath-by-breath by capnographs are not integrated and analyzed together with data coming from other physiologic monitors and lung image analysis, their clinical meaning could be incomplete and even misleading. Modern volumetric capnographs incorporate this physiologic approach, enabling intensivists to measure VD/VTphys at the bedside. Currently, dead space is measured at the bedside by volumetric capnography, which reports expired CO 2 elimination as a function of expired VT, and VD/VTphys is calculated using the Enghoff’s modification of Bohr’s original equation: VD/VTphys = (PaCO 2 – PECO 2)/PaCO 2, where PaCO 2 is the arterial partial pressure of CO 2 obtained by arterial blood sampling and PECO 2 is an estimate of mixed expired partial pressure of CO 2 obtained from the mid-portion of phase III of the volumetric capnogram. 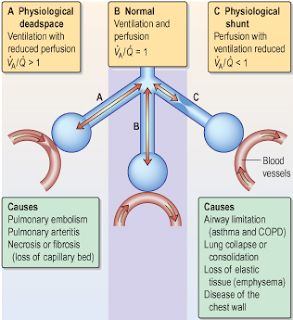
The physiologic ventilatory dead space fraction (VD/VTphys) is usually defined as the fraction of tidal volume (VT) that does not participate in gas exchange. Dead space comprises two separate components: airway dead space (the volume of areas that do not contribute to gas exchange) and alveolar dead space (the volume of well-ventilated alveoli that receive minimal blood flow). Dead space refers to lung areas that are ventilated but not perfused.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
